
Fertility is a complex topic that touches both men and women, yet it is often misunderstood. Misconceptions about fertility are widespread, influenced by myths, social media, anecdotal stories, and outdated medical information.
These misunderstandings can lead to unnecessary stress, poor decision-making, and delays in seeking professional help.
Understanding the facts about fertility can empower individuals and couples to make informed choices about family planning. In this article, we will explore 10 common misconceptions about fertility, providing evidence-based insights and practical advice to help you navigate your reproductive health.
Fertility involves a combination of biological, hormonal, and lifestyle factors, which makes it difficult to fully understand without professional guidance. Some of the reasons fertility myths persist include:

Many fertility beliefs come from outdated research or personal stories, not the latest medical science, causing widespread myths.

Private discussions and social stigma around fertility allow misinformation to spread easily through informal networks.
TV, movies, and social media often oversimplify fertility or show rare cases as typical, creating misleading impressions.

Fertility is complex, influenced by ovulation cycles, sperm quality, hormones, and age, making generalizations unreliable.
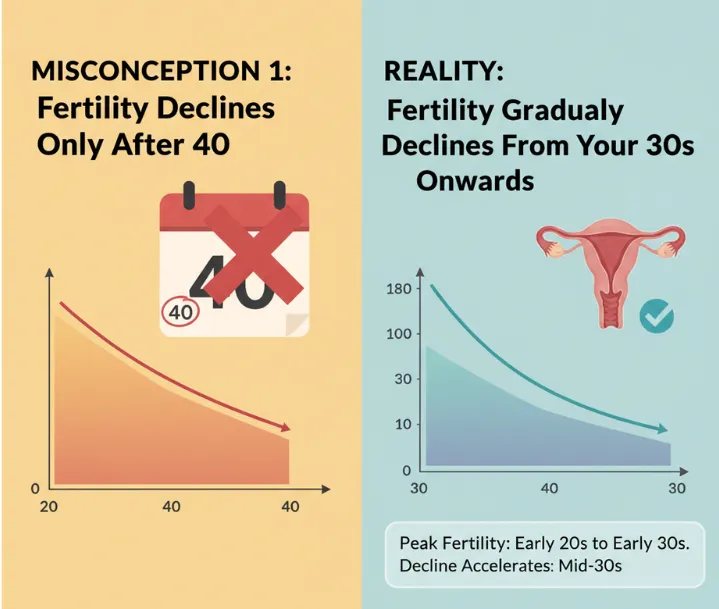
Misconception 1:
Many people believe that women remain fully fertile until they reach their 40s, but fertility actually begins to decline in the late 20s to early 30s.
Understanding that fertility does not remain constant throughout adulthood can help individuals plan earlier, seek fertility testing when needed, and explore options like egg or sperm freezing if family planning is delayed.

Misconception 2:
A healthy lifestyle is important for fertility, but it does not guarantee conception. Nutrition, exercise, and avoiding smoking or excessive alcohol contribute to reproductive health, but other factors may interfere with fertility.
Healthy habits can improve fertility outcomes but should be seen as supportive rather than a guarantee.
Misconception 3:
Fertility is often considered a “woman’s issue,” but male fertility contributes to nearly half of all infertility cases.
Couples struggling to conceive should recognize that fertility evaluation should include both partners, not just women.


Misconception 4:
While menstrual irregularities can indicate hormonal issues, irregular periods do not automatically mean infertility.
It is important to differentiate between irregular menstruation and complete infertility before drawing conclusions.
Misconception 5:
Many people expect pregnancy to occur as soon as they start trying, but conception often takes time.
Understanding that conception can take several months helps reduce unnecessary anxiety and prevents premature assumptions of infertility.


Misconception 6:
In vitro fertilization (IVF) is a powerful fertility treatment but it is not a guaranteed solution.
IVF is a valuable tool for overcoming fertility challenges, but it should be seen as part of a broader treatment plan, not a guaranteed fix.
Misconception 7:
Stress can affect hormone balance and menstrual cycles, but it is rarely the primary cause of infertility.
While stress management is beneficial, it should not be blamed as the main cause of fertility struggles.


Misconception 8:
Many people fear that using birth control pills for years will reduce fertility, but research shows this is largely unfounded.
Birth control is safe for long-term use and does not prevent future pregnancy once discontinued.
Misconception 9:
While healthy habits improve fertility potential, they cannot always reverse infertility caused by medical conditions.
Fertility-friendly habits are important but should complement, not replace, medical evaluation and treatment.


Misconception 10:
Infertility can affect people at any age, not just those over 35. Recognizing that fertility challenges are not limited to older couples helps encourage timely medical consultation.
Fertility myths can create confusion, stress, and delays in seeking appropriate care. Understanding the truth behind common misconceptions empowers individuals and couples to make informed decisions about family planning.
Key takeaways include:
By separating fact from fiction, couples can approach fertility with realistic expectations, reduce stress, and improve their chances of achieving a healthy pregnancy.