
Trying to conceive can feel emotionally overwhelming, especially when it doesn’t happen as quickly as expected. Many couples start worrying, overthinking timing, or feeling pressure from family, age, or personal expectations.
This stress can make an already sensitive journey even harder, and some people may eventually consider visiting a top fertility clinic for guidance.
What many people don’t realize is that mental health and fertility are closely connected. Stress, anxiety, and constant worry can quietly affect hormone balance, ovulation, and even sperm quality, making conception more challenging than it needs to be.
In this article, you’ll get a clear and complete explanation of how stress impacts fertility in both men and women, why it happens, and what practical steps you can take to improve your chances of conception in a healthier and more balanced way.
Fertility depends on a delicate balance of hormones, healthy reproductive organs, and regular ovulation or sperm production.
However, this biological system does not work in isolation. The brain plays a central role in regulating reproductive hormones through the hypothalamus and pituitary gland.
When a person experiences mental stress, the brain releases stress hormones such as cortisol and adrenaline. These hormones can disrupt the normal reproductive signals sent to the ovaries and testes.
Mental health conditions such as anxiety, depression, and chronic stress can therefore indirectly influence fertility by interfering with hormonal communication and reproductive function.

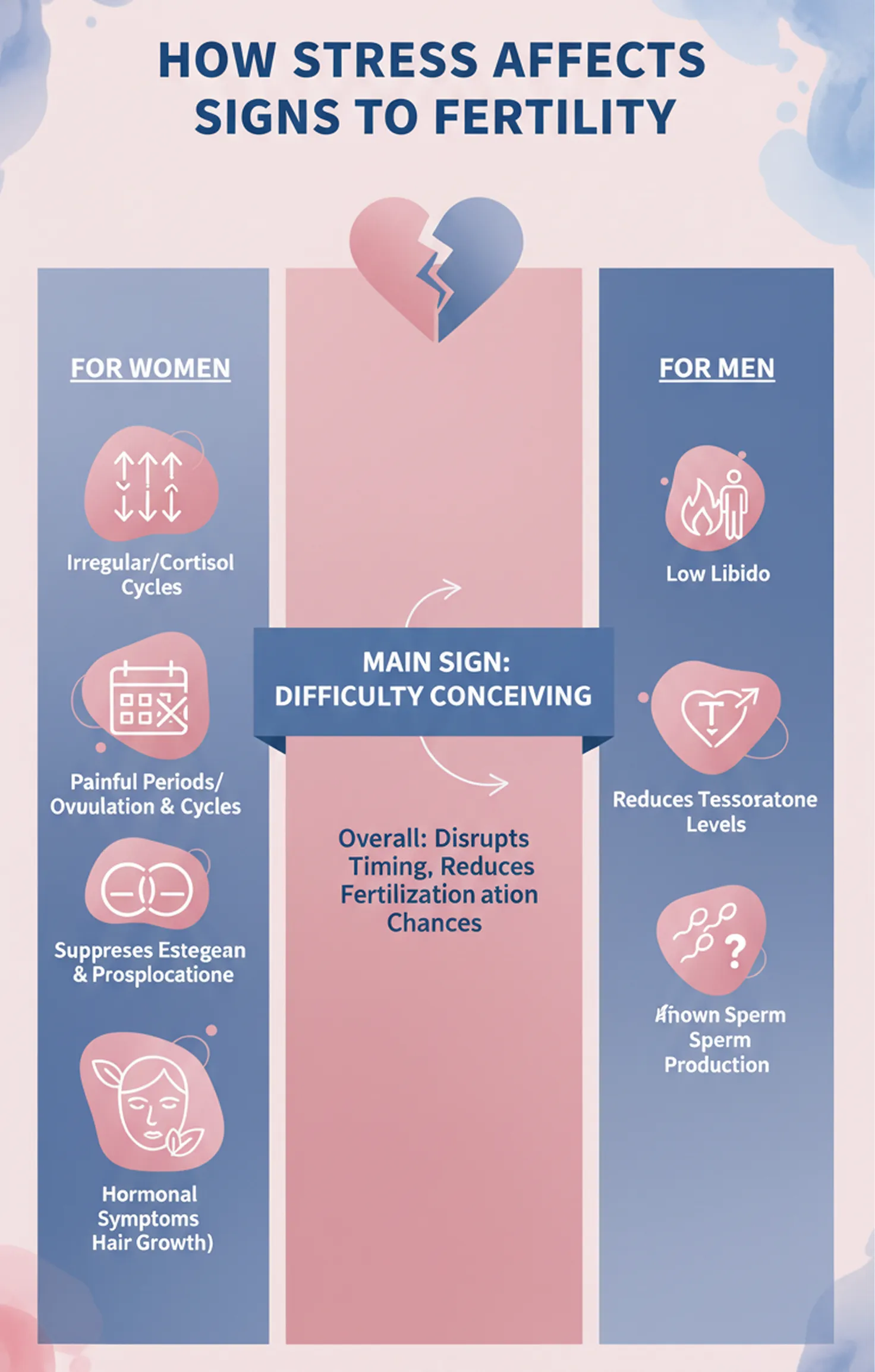
Stress activates the body’s “fight or flight” response.
While this is helpful in short-term danger situations, long-term stress can cause hormonal imbalance.
Here is how stress affects fertility:
When stress becomes chronic, the body prioritizes survival functions over reproduction.
This is why conception can become more difficult during emotionally or physically stressful periods.
Not all stress is the same.
Different types can affect fertility in different ways, especially when experienced over a long period:

Mental health can also create invisible barriers to conception. Couples trying to conceive may experience:
These psychological factors can reduce sexual frequency, lower desire, and increase stress levels, creating additional challenges for natural conception.
Women experiencing high stress may notice changes in libido, sleep quality, and energy levels, all of which are important for reproductive health.
In women, stress can affect fertility in several ways:
Chronic stress may also affect the uterine lining, making it less receptive for embryo implantation.
This can reduce the chances of pregnancy even when ovulation occurs normally.

Unlike women, sperm production is continuous, but stress can still affect the quality of sperm produced over a period of weeks or months. Male fertility is also sensitive to stress. High stress levels can lead to:
Stress can also affect sexual performance, leading to erectile difficulties or reduced sexual interest. Over time, these issues can significantly lower the chances of conception.
One of the biggest challenges in fertility and mental health is the “fertility-stress cycle.”
It works like this:
This cycle can continue unless it is consciously addressed.
Breaking this pattern is often essential for improving fertility outcomes naturally.

Research shows a clear connection between stress and reproductive health, although stress alone is rarely the only cause of infertility.
Studies suggest that:
While fertility is influenced by many medical factors, emotional well-being is now considered an important supporting element in reproductive health care.

Managing stress is not about eliminating it completely but about controlling its impact on the body.
Some effective approaches include:
Even small daily habits that reduce stress can positively influence hormonal balance over time.

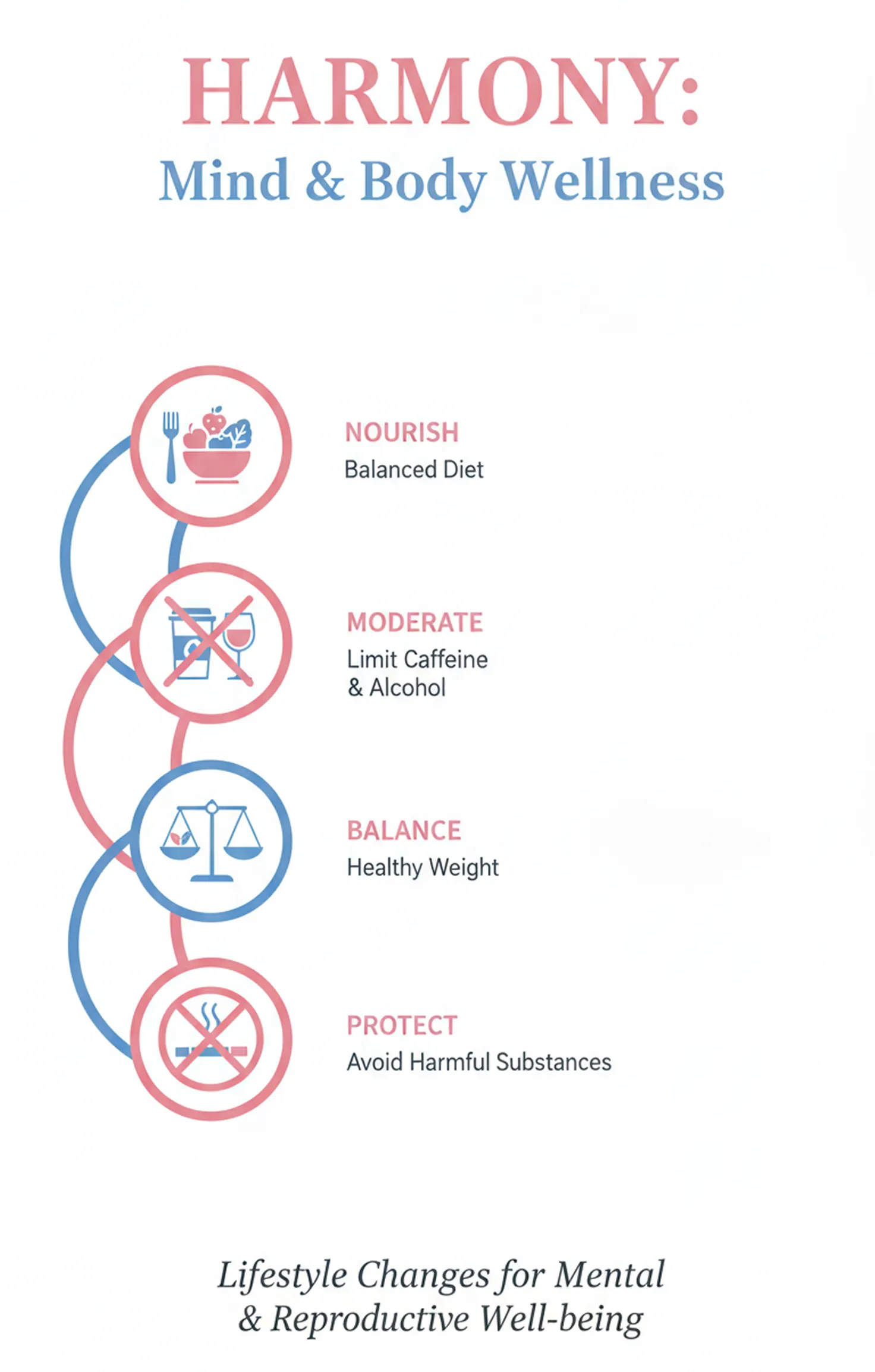
Lifestyle plays a major role in both stress management and fertility. Helpful changes include:
These changes support both brain health and reproductive function, improving the chances of conception naturally.
In some cases, medical support may be necessary alongside stress management. Fertility specialists may recommend:
Combining medical treatment with emotional support often provides better outcomes than focusing on either alone.
A balanced approach is often the most effective. Some best practices include:
A calm and supportive environment can significantly improve both emotional well-being and reproductive health.

Stress and fertility are closely connected through complex hormonal and psychological pathways. While stress does not always directly cause infertility, it can influence reproductive function in both men and women.
The good news is that stress is manageable. Through lifestyle changes, emotional support, and proper medical guidance when needed, many couples can improve their chances of conception.
Understanding the link between mental health and fertility helps reduce unnecessary pressure and creates a healthier, more balanced path toward pregnancy.